I Spent 3 Years Trying to Lose My Belly Fat. Then My Doctor Told Me to Stop Dieting.
New research is overturning decades of weight loss advice for women over 35. Here's what's actually happening inside your body — and why the answer isn't another diet.


Jennifer Marsh, 44, was doing everything her doctor told her to do.
She ate clean. She did Pilates four times a week. She was in bed by 10 PM. She cut out alcohol, tracked her macros, and drank more water than she thought was physically possible.
And yet, for three years, the belly fat didn't move.
"My doctor kept telling me to eat less and move more," she told me when we spoke last spring. "But I was already doing both. I started to think I was just broken."
She's not broken. And she's not alone.
According to a 2023 study published in the Journal of Clinical Endocrinology & Metabolism, more than 68% of women between the ages of 35 and 55 who report persistent abdominal weight gain despite caloric restriction show measurably elevated cortisol levels — often two to three times the normal range.
Then, at a routine blood panel, Jennifer's doctor noticed something that changed everything.
The Number That Changed Everything
Her cortisol was running at nearly three times the normal range.
"I asked her what that meant," Jennifer said. "She told me: 'Your body thinks it's in a famine. It's storing fat to survive. And every diet you try is making it worse.'"
'Your body thinks it's in a famine. It's storing fat to survive. And every diet you try is making it worse.'
Cortisol is your body's primary stress hormone. In short bursts, it's essential — it helps you respond to danger, regulate blood sugar, and manage inflammation. But when cortisol stays elevated for weeks or months, something goes wrong.
Your body interprets chronic high cortisol as a signal of prolonged scarcity. So it does what it evolved to do: it slows your metabolism, increases your appetite for calorie-dense foods, and — critically — it directs fat storage specifically to the abdomen, where it can be quickly accessed in an emergency.
This is why women with high cortisol often have a very specific body composition: slim arms and legs, but a persistent belly that won't respond to diet or exercise.
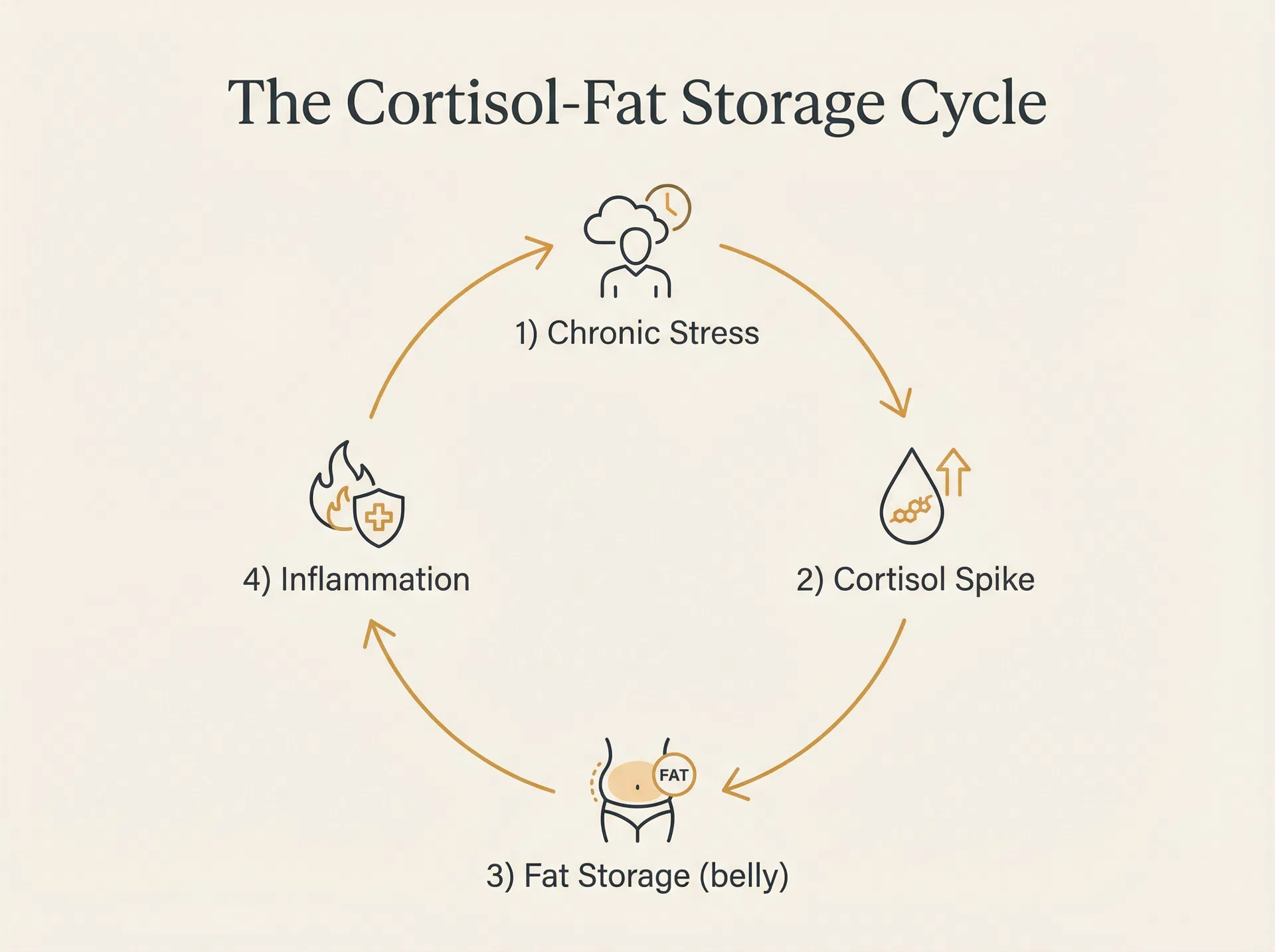
But here's what Jennifer's doctor told her next — and it surprised her most.
Why "Eat Less, Move More" Is Making It Worse
Caloric restriction is a stressor. Your body doesn't know the difference between a voluntary diet and an actual famine. When you cut calories significantly, cortisol goes up. When you do intense cardio — the kind most women turn to when they're frustrated — cortisol spikes again.
In other words: the very interventions that are supposed to help are, for women with elevated cortisol, actively making the problem worse.
"I've had patients who were eating 1,200 calories a day and doing cardio six days a week and still gaining weight," says Dr. Marcus Webb, a functional medicine physician based in Austin who specializes in hormonal health. "When I test their cortisol, it's always through the roof. The diet is the problem, not the solution."
So what actually works?
The answer, it turns out, is in a 3,000-year-old spice.
The Compound Most Doctors Have Never Heard Of
Saffron — the spice derived from the Crocus sativus flower — has been used in Persian medicine for millennia to treat anxiety, mood disorders, and what ancient physicians called "melancholy of the stomach."
Modern researchers, intrigued by these historical uses, began investigating the active compounds in saffron in the early 2000s. What they found was unexpected.
The primary active compound, safranal, appears to directly modulate the hypothalamic-pituitary-adrenal (HPA) axis — the system that regulates cortisol production. In plain English: saffron tells your body to stop producing so much cortisol.
A 2021 randomized controlled trial published in Phytotherapy Research found that women who supplemented with 88.5mg of saffron extract daily for 12 weeks showed a 36% reduction in morning cortisol levels compared to placebo. They also reported significantly reduced food cravings, improved sleep quality, and measurable reductions in abdominal fat circumference.
There's also a bioavailability problem. Saffron's active compounds are fat-soluble, which means they need fat to be absorbed properly. Without a bioavailability enhancer — most commonly piperine, derived from black pepper — the majority of the saffron passes through the digestive system without being absorbed.
Jennifer's doctor knew all of this. And she recommended one specific formula.
What Jennifer's Doctor Recommended
The formula is called Saffron Complete, made by a company called Methodic Bio.

It's not a weight loss pill. The company is careful about that distinction. It's a cortisol regulation formula — nine ingredients, each chosen for a specific role in the cortisol-fat storage cycle.
The saffron extract is dosed at 88.5mg — the clinical trial dose. It's combined with ashwagandha (which has its own body of evidence for cortisol reduction), L-theanine (which promotes calm without sedation), magnesium glycinate (depleted by chronic stress), and piperine to ensure absorption.
"This isn't about suppressing hunger or burning fat directly," Dr. Webb explained. "It's about addressing the upstream cause. When cortisol normalizes, the body stops defending the belly fat. That's when diet and exercise actually start working."
'When cortisol normalizes, the body stops defending the belly fat. That's when diet and exercise actually start working.'
Jennifer started taking Saffron Complete in February of last year. She didn't change her diet. She didn't add more exercise.
At 30 days, she noticed her sleep had improved and her afternoon cravings had largely disappeared. At 60 days, her pants were looser. At 90 days, she had lost 11 pounds — almost entirely from her midsection.
"I've been trying to lose this weight for three years," she said. "And in three months, it just started coming off. I wasn't doing anything differently except taking this."
What You Should Know Before Trying It
This is not a miracle. There are a few things worth understanding before you consider trying Saffron Complete.
First, the timeline. The research suggests that meaningful cortisol reduction takes 8–12 weeks of consistent supplementation. This is not a product you take for two weeks and expect dramatic results. The women in the clinical trials who saw the most significant outcomes were consistent for a full 90 days.
Second, it works best when cortisol is actually the problem. If your belly fat is purely the result of caloric excess or inactivity, this formula is not going to be the answer. But if you recognize yourself in Jennifer's story — doing everything right and still not seeing results — cortisol dysregulation is worth investigating.
Third, quality matters enormously. The saffron market is flooded with underdosed, poorly-sourced products. Methodic Bio is one of the few companies using the clinical trial dose with third-party testing. That's why this specific formula is the one that keeps appearing in functional medicine conversations.
What Our Readers Are Saying
Since we first covered the cortisol-belly fat connection six months ago, we've received hundreds of letters from readers. Here are three that we found particularly representative.
"I've been on every diet imaginable since my late 30s. Nothing stuck. My doctor suggested I get my cortisol tested after reading your article, and it was elevated. I've been on Saffron Complete for 10 weeks and I've lost 8 pounds without changing anything else. I'm honestly still in shock."
— Diane R., Nashville, TN
"I was skeptical. I've been burned by supplements before. But the research you cited was real — I looked it up myself. I'm at week 7 now and my sleep is dramatically better. The belly fat is moving slowly but it's moving. That's more than I can say for the last two years."
— Michelle T., Portland, OR
"What got me was the part about caloric restriction making cortisol worse. I've been in a 1,200-calorie deficit for six months and I've actually gained weight around my middle. My functional medicine doctor confirmed my cortisol is high. Starting Saffron Complete this week."
— Karen L., Atlanta, GA
Methodic Bio has authorized a limited inventory allocation for readers in the United States.
This price is not available on their website or at any retailer. The allocation for United States readers expires today, April 6, 2026, at 11:59 PM.
A Final Note
Jennifer Marsh is not a special case. She is, in many ways, the average American woman over 40 — health-conscious, motivated, and completely confused about why her body isn't responding to her efforts.
The cortisol connection is not new science. It's been in the research literature for decades. What's new is the growing recognition that for a significant subset of women, cortisol dysregulation is the primary driver of abdominal weight gain — and that addressing it directly, rather than through more aggressive dieting, is the more effective path.
Whether that means Saffron Complete specifically, or simply getting your cortisol tested and working with a functional medicine physician, the first step is the same: stop assuming the problem is effort, and start asking whether it might be hormonal.
Jennifer put it simply when we ended our conversation: "I wish someone had told me this three years ago."
About the Author: Sarah Chen is a health and science reporter who has covered functional medicine and women's hormonal health for eight years. She holds a master's degree in science journalism from Northwestern University.
Disclosure: This article contains a sponsored offer from Methodic Bio. The editorial content and research cited are independent of the commercial arrangement.
© 2026 Integrative Health Today. All rights reserved.